 Metabolic syndrome is a group of conditions that increase the risk of heart disease, stroke, type 2 diabetes, and other health problems.
Metabolic syndrome is a group of conditions that increase the risk of heart disease, stroke, type 2 diabetes, and other health problems.
The number of people with metabolic syndrome is increasing, as up to one-third of adults in the U.S. have it.
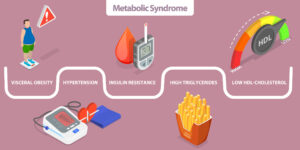
When a person is diagnosed with metabolic syndrome, they have three or more risk factors, such as:
- High blood pressure
- High blood sugar
- Low levels of HDL, or good cholesterol
- High triglyceride levels in the blood
- A large waist circumference or an apple-shaped body
Although each of these conditions is a risk factor for cardiovascular disease, when a person has three or more of them and is diagnosed with metabolic syndrome, the chances of them developing a serious cardiovascular condition increase.
There are several underlying causes of metabolic syndrome, such as:
- Being overweight and being obese
- Having an insulin resistance
- Being physically inactive
- Genetic factors
- Increasing age
Metabolic syndrome is a serious health condition; however, there are ways to reduce your risk of developing it, such as:
- Being more physically active
- Losing weight
- Eating a heart-healthy diet that is rich in:
- Whole grains
- Fruits and vegetables
- Fish
Another way to reduce your risk of developing metabolic syndrome is working with your healthcare team to monitor and manage your blood sugar, blood cholesterol, and blood pressure.
If you or a loved one is experiencing symptoms of metabolic syndrome, you can receive treatment at Flushing Hospital Medical Center’s Ambulatory Care Center. To schedule an appointment, please call (718) 670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.










