 Basilar invagination is a rare condition that occurs when the top of the spine gets pushed into the base of the skull. This can lead to pinching or pressure on the brainstem, which is the group of nerves connecting the brain to the spinal cord. This condition is painful and can cause various neurological symptoms.
Basilar invagination is a rare condition that occurs when the top of the spine gets pushed into the base of the skull. This can lead to pinching or pressure on the brainstem, which is the group of nerves connecting the brain to the spinal cord. This condition is painful and can cause various neurological symptoms.
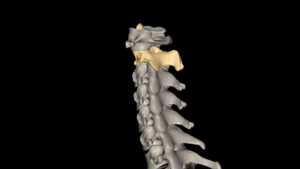
The spine is made of seven vertebrae and is numbered from C1 to C7; this is called the cervical vertebrae. The C1 vertebrae is at the top of the spine, supporting the skull. The C2 vertebrae lies below the C1 and has an upward peg that enters a hole in the C1, which lets the C1 vertebrae pivot on the C2, allowing the head to turn sideways.
If the peg of the C2 vertebra moves too far upward into the C1 vertebra, it can put pressure on the brainstem. The brainstem normally passes from the skull into the spinal canal through an opening at the base of the skull called the foramen magnum.
In basilar invagination, the C2 vertebra moves upward toward this opening. As it pushes into the foramen magnum, the space for the brainstem becomes smaller. This reduced space can lead to compression of the brainstem.
Basilar invagination occurs when a person has problems with the bones in the neck or vertebrae. It can also be caused by platybasia, which is the flattening of the base of the skull. Basilar invagination can be present at birth. However, it can develop later due to illness or injuries resulting from vehicle or bicycle accidents, falls, or accidents during activities such as diving.
Basilar invagination may occur in people with conditions, such as:
- Rheumatoid arthritis
- Tumors
- Paget’s disease
- Brittle bone disease
- Marfan syndrome
- Rickets
The symptoms of basilar invagination can vary based on the pressure on the brainstem, spinal cord, or nerves. Symptoms may become noticeable when a person bends their neck. Symptoms of basilar invagination include:
- Headache or pain in the back of the head
- Weakness in the neck, arms, and legs
- Tingling when bending the neck
- Tingling or numbness in the hands or feet
- Difficulty swallowing or talking due the loss of muscle control caused by nerve damage
- Inability to tell the position of body parts without looking
- Twitching eye movements or nystagmus
- Loss of feeling or sensation in limbs
- Dizziness or lightheadedness
- Confusion
A person may also feel a shock down their back when they bend their neck forward or may experience paralysis.
If basilar invagination goes untreated, it can cause complications such as hydrocephalus or syringomyelia, which are conditions that occur when the flow of fluid around the brain and spinal cord is blocked and the fluid collects in the brain or spinal cord. What’s more, if the lower brainstem gets compressed, it may result in death.
Basilar invagination is diagnosed when a healthcare provider performs an examination to look for symptoms of the condition as well as discusses a person’s medical history. They will also use tests to check if a person’s spine and nerves are affected. These tests include:
- X-rays
- MRI
- CT scan
- Myelography
- Nerve conduction studies
The treatment for basilar invagination depends on its symptoms and severity of the condition. If a person has basilar invagination that presents without signs of brainstem compression pressure on the spinal cord, a healthcare provider will use:
- Non-steroidal anti-inflammatory drugs (NSAIDs) such as aspirin to relieve pain or swelling
- Neck traction, which involves gently stretching the neck to increase the space between the bones to relieve pressure
- A neck collar or brace to support the neck and limit movement
- Physical therapy that consists of neck exercises
If a person has signs of brainstem compression and nerve problems, they will need surgery. Surgery can be performed through the nose or mouth and can also be performed at the junction of the head and neck. Healthcare providers aim to use surgery to decompress or relieve the pressure on the brainstem or spinal cord and stabilize the joint in the neck.
If you or a loved one is experiencing symptoms associated with basilar invagination, you can receive treatment at Flushing Hospital Medical Center’s Ambulatory Care Center. To schedule an appointment, please call (718) 670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.