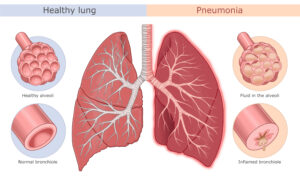
 Pneumonia is an infection that inflames the air sacs in one or both lungs. The air sacs may fill with fluid or pus, causing a cough with phlegm or pus, fever, chills, and difficulty breathing.
Pneumonia is an infection that inflames the air sacs in one or both lungs. The air sacs may fill with fluid or pus, causing a cough with phlegm or pus, fever, chills, and difficulty breathing.
Pneumonia can range in severity from mild to life-threatening. It is more serious for infants and young children, people older than 65 years old, and people with health problems or weakened immune systems.
The signs and symptoms of pneumonia can vary depending on factors such as the type of germ causing the infection, age, and overall health. Signs and symptoms of pneumonia may include:
- Chest pain when breathing or coughing
- Confusion or changes in mental awareness; this occurs in adults 65 or older
- A phlegm-producing cough
- Fatigue
- Fever, sweating, and shaking chills
- Lower than normal body temperature; this occurs in adults older than 65 and people with weakened immune systems
- Nausea, vomiting, or diarrhea
- Shortness of breath
Many germs can cause pneumonia. The most common are bacteria and viruses in the air we breathe. The body usually prevents these germs from infecting the lungs, but these germs can sometimes overpower the immune system, even if a person is generally healthy.
Pneumonia is classified according to the types of germs that cause it and where the infection was contracted.
Community-acquired pneumonia is the most common type of pneumonia. It occurs outside of hospitals or other healthcare facilities. It may be caused by:
- Bacteria
- Bacteria-like organisms
- Fungi
- Viruses, such as COVID-19
Some people can get pneumonia during a hospital stay for another illness. Hospital-acquired pneumonia can be serious because the bacteria causing it may be more resistant to antibiotics and because the people who get it are already sick. People who are on breathing machines, often used in intensive care units, are at a higher risk of this type of pneumonia.
Healthcare-acquired pneumonia is a bacterial infection that occurs in people who live in long-term care facilities or who receive care in outpatient clinics, including kidney dialysis centers. Like hospital-acquired pneumonia, healthcare-acquired pneumonia can be caused by bacteria that are more resistant to antibiotics.
Aspiration pneumonia occurs when a person inhales food, a drink, vomit, or saliva into their lungs. Aspiration is more likely if something disturbs the normal gag reflex, such as a brain injury or swallowing problem, or excessive use of alcohol or drugs.
There are many steps you can take to prevent pneumonia, including:
- Getting vaccinated
- Making sure children are vaccinated
- Practicing good hygiene
- Quitting smoking
- Keeping your immune system strong
To diagnose pneumonia, a doctor will start by asking about your medical history and performing a physical exam, including listening to your lungs with a stethoscope to check for abnormal bubbling or crackling sounds that may suggest pneumonia.
If pneumonia is suspected, a doctor may recommend the following tests:
- Blood tests
- Chest X-ray
- Pulse oximetry
- Sputum test
A doctor might order additional tests for a person 65 years or older, is in the hospital, or has serious symptoms or health conditions. These tests may include a CT scan and/or a pleural fluid culture.
Treatment for pneumonia involves curing the infection and preventing complications. People who have contracted community-acquired pneumonia usually can be treated at home with medication. Although most symptoms ease in a few days or weeks, the tiredness feeling can persist for a month or more. Specific treatments depend on the type and severity of pneumonia, age, and overall health. These treatments include:
- Antibiotics
- Cough medicine
- Fever reducers/pain relievers
If you or a loved one is experiencing symptoms of pneumonia, you can receive treatment from a physician at Flushing Hospital Medical Center’s Ambulatory Care Center. To schedule an appointment, please call (718) 670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.