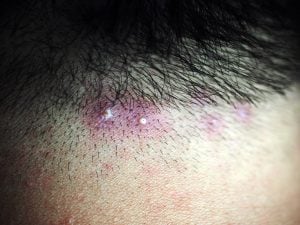
 Folliculitis is a common skin condition in which hair follicles become infected or inflamed.
Folliculitis is a common skin condition in which hair follicles become infected or inflamed.
Folliculitis can look similar to acne and be uncomfortable or itchy, and because of its appearance, it can often have a psychosocial impact.
The two main forms of folliculitis are superficial and deep. The superficial form involves part of the follicle, while the deep form involves the entire follicle and is usually more severe.
There are many different types of folliculitis. Each type is unique based on the cause, the infectious organism, and its impact on the skin. The different types of folliculitis include:
- Bacterial folliculitis
- Hot tub rash
- Malassezia folliculitis
- Razor bumps
- Sycosis barbae
- Gram-negative folliculitis
- Boils
- Carbuncles
- Eosinophilic folliculitis
Folliculitis appears anywhere on the body that has hair, such as the face, arms, upper back, and lower legs. Hair follicles can gather bacteria and other materials from the outside world that could cause inflammation or infection. When something is inflamed, it is swollen. A swollen hair follicle will bulge up and make a bump on the skin. If you have an infected hair follicle, you may experience:
- Redness
- Irritation
- Itching
- Bumps on the skin
Folliculitis is caused when a hair follicle is inflamed or infected with bacteria, commonly Staphylococcus aureus. This causes the follicle to swell under the skin, creating uncomfortable bumps on the surface. For many specific types of folliculitis, the cause isn’t always known. However, certain factors can increase the risk of developing this condition, including:
- If you shave often
- If you have been using an oral antibiotic for a long time
- If you are overweight or obese
- If you do activities that make you sweat a lot and don’t fully clean off afterward
- If you spend time in a hot tub or sauna that isn’t properly cleaned
Signs and symptoms of folliculitis include:
- Clusters of small bumps of pimples around hair follicles
- Pus-filled blisters that break open and crust over
- Itchy, burning skin
- Painful, tender skin
- An inflamed bump
To diagnose folliculitis, a healthcare provider will examine your skin and ask about your medical history. If early treatments don’t clear up the infection, the healthcare provider will run tests, including:
- Scraping the skin to look for yeast under the microscope
- They may take a swab for culture to determine the cause of the infection
- In rare cases, they may do a skin biopsy to rule out other conditions
Treatment for folliculitis depends on the type and severity of the condition, what self-care measures were tried, and how you would like to proceed.
If you have tried nonprescription products for a few weeks and they haven’t helped, ask a healthcare provider about prescription-strength medications. A dermatologist can help you:
- Control your folliculitis
- Figure out whether a drug you take might be causing your symptoms and whether you can stop taking it
- Avoid scarring or other damage to the skin
- Make scars less noticeable
There are many ways that you can prevent folliculitis, including the following:
- Washing your skin regularly
- Doing laundry regularly
- Avoiding friction or pressure on your skin
- Avoiding shaving, if possible
- Shaving with care
- Trying hair-removing products or other methods of hair removal
- Treating related conditions
- Using only clean hot tubs and heated pools
Sometimes, folliculitis goes away without medical treatment. Self-care measures such as applying a warm, moist washcloth to the affected skin followed by an anti-itch cream may help relieve your symptoms.
If you have symptoms of folliculitis, you can receive treatment at Flushing Hospital Medical Center’s Ambulatory Care Center. To schedule an appointment, please call (718) 670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.