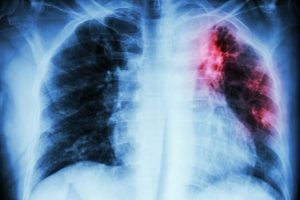
 Tuberculosis is a serious infectious disease that mainly affects the lungs. It is caused by a bacteria called Mycobacterium tuberculosis. Tuberculosis can spread when a person with the illness coughs, sneezes, or speaks, releasing tiny droplets of germs into the air. Another person can breathe in the droplets, and the germs will enter the lungs.
Tuberculosis is a serious infectious disease that mainly affects the lungs. It is caused by a bacteria called Mycobacterium tuberculosis. Tuberculosis can spread when a person with the illness coughs, sneezes, or speaks, releasing tiny droplets of germs into the air. Another person can breathe in the droplets, and the germs will enter the lungs.
When tuberculosis germs survive and multiply in the lungs, it is a TB infection. A TB infection can happen in one of three stages, each with symptoms.
Primary TB infection is the first stage of TB infection. Immune system cells find and capture the germs, which the immune system may destroy. However, some captured germs can still survive and multiply.
Most people don’t have symptoms during primary infection. Some people may have flu-like symptoms, including:
- Low fever
- Tiredness
- Cough
Latent TB infection is the stage following primary TB infection. Immune system cells build a wall around lung tissue with TB germs, which keeps them under control. However, the germs survive. There aren’t any symptoms during latent TB infection.
Active TB disease happens when the immune system can’t control an infection. Germs cause disease throughout the lungs or other parts of the body. Active TB disease can happen right after primary infection, but it usually occurs after months or years of latent TB infection. Symptoms of active TB disease in the lungs begin gradually and worsen over a few weeks. Symptoms can include:
- Cough
- Coughing up blood or mucus
- Chest pain
- Pain with breathing or coughing
- Fever
- Chills
- Night sweats
- Weight loss
- Loss of appetite
- Tiredness
- Not feeling well in general
Extrapulmonary tuberculosis occurs when an active TB infection spreads from the lungs to other body parts. Symptoms vary depending on what part of the body is infected. Common symptoms can include:
- Fever
- Chills
- Night sweats
- Weight loss
- Not wanting to eat
- Tiredness
- Not feeling well in general
- Pain near the site of infection
Common sites of active TB disease outside of the lungs include:
- Kidneys
- Liver
- Fluid surrounding the brain and spinal cord
- Heart muscles
- Genitals
- Lymph nodes
- Bones and joints
- Skin
- Walls of blood vessels
- The voice box or larynx
People with active TB infection can spread tuberculosis easily, especially in crowded spaces.
To diagnose a TB infection, a healthcare provider will perform an exam that includes:
- Listening to you breathe with a stethoscope
- Checking for swollen lymph nodes
- Asking you questions about your symptoms
Your healthcare provider will order tests if:
- Tuberculosis is suspected
- You were likely exposed to a person with active TB disease
- You have health risks for active TB disease
Your healthcare provider will determine whether a skin or blood test is best. X-rays, sputum tests, and other lab tests can also diagnose a TB infection.
Your healthcare provider may treat you with drug treatments if you have a latent TB infection. This is especially true for people who are at an increased risk of active TB disease. Most latent TB infections are treated for three or four months. Active TB may be treated for four, six, or nine months. Specialists in TB treatment will determine which drugs are best for you.
It is important to take every dose as instructed when your healthcare provider prescribes medication. You must complete the full course of treatment, as it is important for killing the bacteria in your body and preventing new drug-resistant bacteria.
If you are experiencing symptoms of tuberculosis, you must receive treatment from a doctor as soon as possible. You can schedule an appointment at Flushing Hospital Medical Center’s Ambulatory Care Center by calling (718) 670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.