Mpox previously known as monkeypox, is a viral illness caused by the monkeypox virus. The virus usually affects rats, mice, or monkeys. But it can occur in people as well.
Mpox previously known as monkeypox, is a viral illness caused by the monkeypox virus. The virus usually affects rats, mice, or monkeys. But it can occur in people as well.
Mpox usually occurs in Central and West Africa. Cases outside of Africa are due to international travel, imported animals, and close contact with an animal or person infected with mpox.
Mpox symptoms may start three to 17 days after exposure. Symptoms last two to four weeks and may include:
- Fever
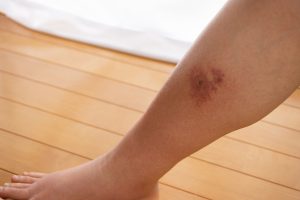
- Skin rash
- Swollen lymph nodes
- Headache
- Muscle aches and backaches
- Chills
- Fatigue
A skin rash starts about one to four days after a fever. It first appears on the face, hands, or feet and then spreads to other body parts. You can spread mpox while you have symptoms.
There are many ways that mpox can spread, including:
- Person to person
- Direct contact with rashes, scabs, or bodily fluids of a person with mpox
- Extended close contact with respiratory droplets from an infected person, including sexual contact
- Clothes, sheets, blankets, or other materials that have been in contact with rashes or bodily fluids of an infected person
- An infected pregnant person can spread the mpox virus to a fetus
- Animal to person
- Animal bites or scratches
- Wild game that is cooked for food
- Products, such as skins or furs made from infected animals
- Direct contact with bodily fluids or rashes of animals with mpox
There are many steps you can take to prevent infection or the spread of the mpox virus, including:
- Avoiding close contact with people who have a rash that looks like mpox
- Avoiding the handling of clothes, sheets, blankets, or other materials that have been in close contact with an infected animal or person
- Quarantining people who have mpox from healthy people
- Washing your hands well with soap and water after contact with an infected person or animal. If soap and water aren’t available, use an alcohol-based hand sanitizer
- Avoiding animals that may carry the virus
The treatment for most people with mpox is aimed at relieving symptoms. Care may include managing skin damage from the mpox rash, drinking enough fluids to help keep stool soft, and pain management. There is no specific treatment approved for mpox. Healthcare professionals may treat mpox with antiviral drugs used to treat smallpox. If you have mpox, quarantine at home in a room separate from family and pets until your rash and scabs heal.
You can make an appointment for mpox treatment and prevention at Flushing Hospital Medical Center’s on-site ambulatory care center by calling (718) 670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.