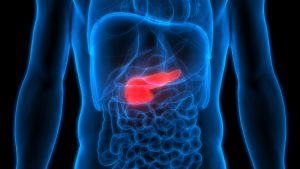
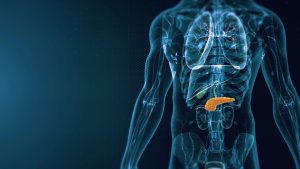
 Pancreatitis is the inflammation or swelling of the pancreas. This may happen when digestive juices or enzymes attack the pancreas. The pancreas is a gland on the left side of your belly that lies behind your stomach. The pancreas’ two main functions are:
Pancreatitis is the inflammation or swelling of the pancreas. This may happen when digestive juices or enzymes attack the pancreas. The pancreas is a gland on the left side of your belly that lies behind your stomach. The pancreas’ two main functions are:
- To make enzymes to send to your small intestines. These enzymes help break down food.
- To make hormones insulin and glucagon, sending them into your bloodstream. These hormones control your body’s blood sugar level.
Pancreatitis can be either acute or chronic. Signs and symptoms of acute pancreatitis include:
- Pain in the upper belly
- Pain in the upper belly that radiates to the back
- Tenderness when touching the belly
- Fever
- Rapid pulse
- Upset stomach
- Vomiting
Signs and symptoms of chronic pancreatitis include:
- Pain in the upper belly
- Belly pain that feels worse after eating
- Losing weight without trying
- Oily, smelly stools
Several conditions can lead to acute pancreatitis, including:
- Blockage in the bile duct caused by gallstones
- Heavy alcohol use
- Certain medicines
- High triglyceride levels in the blood
- High calcium levels in the blood
- Pancreatic cancer
- Injuries from trauma or surgery
Conditions that can lead to chronic pancreatitis include:
- Damage from repeated acute pancreatitis
- Heavy alcohol use
- Inherited genes linked to pancreatitis
- High triglyceride levels in the blood
- High calcium levels in the blood
Sometimes a cause for pancreatitis is never found. This is called idiopathic pancreatitis.
Many factors can increase your risk of pancreatitis, including:
- Excessive alcohol use
- Cigarette smoking
- Obesity
- Diabetes
- Family history of pancreatitis
Pancreatitis can cause several serious complications that include:
- Kidney failure
- Breathing problems
- Infection
- Pseudocyst
- Malnutrition
- Diabetes
- Pancreatic cancer
When diagnosing pancreatitis, your healthcare provider will ask questions about your health history and symptoms, give you a general physical, and check for pain or tenderness in your belly. They may also administer tests and procedures including:
- Blood tests
- Ultrasounds
- CT scans
- MRIs
- Endoscopic ultrasound
- Stool tests
There is no specific medicine to treat pancreatitis. Treatment will begin with a hospital stay to manage any symptoms and complications. Treatment can include:
- Pain medicines
- Intravenous fluids
- Nutrition plans
When the symptoms and complications are under control, other treatments are used to treat any underlying causes, including:
- Procedures to open bile ducts
- Gallbladder surgery
- Pancreas procedures
- Treatment for alcohol dependence
- Changes in medicine
If you or anyone you know is experiencing signs or symptoms of pancreatitis, you can schedule an appointment with a gastroenterologist at Flushing Hospital’s Ambulatory Care Center, by calling 718-670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.