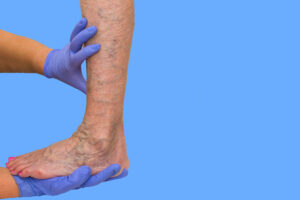
 Chronic venous insufficiency (CVI) is a form of venous disease that occurs when the veins in the legs become damaged and do not work properly.
Chronic venous insufficiency (CVI) is a form of venous disease that occurs when the veins in the legs become damaged and do not work properly.
Normally, the valves in the legs keep blood flowing back up to the heart. CVI damages those valves, causing blood to pool in the legs, increasing pressure in the veins, and causing symptoms such as swelling and ulcers.
Chronic venous insufficiency can happen due to damage to any of the leg veins. These can include:
- Deep veins, which are the large veins deep in the body that run through muscle
- Superficial veins, which are close to the skin’s surface
- Perforating veins, which connect the deep and superficial veins
CVI may cause mild symptoms at first. However, this condition can interfere with a person’s quality of life and lead to serious complications over time. There are several signs and symptoms of chronic venous insufficiency, including:
- Legs that feel tired or achy
- A burning or prickly feeling in the legs
- Reddish brown colored skin
- Varicose veins
- Flaking or itching on the legs or feet
- The feeling of fullness or heaviness in the legs
- Cramping in the legs at night
- Swelling in the lower legs and ankles, especially after standing for a while or at the end of the day
- Leathery-looking skin on the legs
- Ulcers that form near the ankles, which can become infected and painful
Chronic venous insufficiency usually affects people over the age of 50. The risk of developing the disease rises the older a person gets. Overall, chronic venous insufficiency affects about one in 20 adults.
Venous disorders are a general category for many possible vein issues, including CVI. They have various stages that are based on clinical signs, which a healthcare provider can see or feel when they examine your legs. The stages of venous disorders range from 0 to 6. These stages include:
- Stage 0: There are no visible signs; however, a person may feel fatigued or achy
- Stage 1: superficial veins, such as spider veins, are visible
- Stage 2: varicose veins that are at least three millimeters wide
- Stage 3: swollen limbs that don’t have any changes to the skin
- Stage 4: changes to the color and/or texture of the skin
- Stage 5: an ulcer that has healed
- Stage 6: an open ulcer
Chronic venous insufficiency is diagnosed at stage 3 or above.
There are three causes of valve malfunction: congenital, primary, or secondary.
- Congenital causes of valve malfunction are deformities in the leg veins that a person is born with. Some people can be born without valves in their legs
- Primary causes of valve malfunction are any changes to the leg veins that stop them from working correctly. A vein may get too wide, preventing its valve from completely closing
- Secondary causes of valve malfunction are other types of medical issues that damage the leg veins. This is usually caused by deep vein thrombosis (DVT), the most common cause of CVI. The blood clot, or thrombus, leaves behind scar tissue, damaging the valve
Chronic venous insufficiency is diagnosed through a physical exam and ultrasound imaging.
Treatment for CVI involves lifestyle changes, such as leg elevation, exercise, weight management, and compression therapy. If these measures are not enough, a healthcare provider may recommend a procedure or surgery. The best treatment depends on how far the condition has progressed and the other medical conditions a person has.
The goals of treatment are to help the blood flow better through the veins, help ulcers heal and limit their chances of returning, improve the skin’s appearance, and reduce pain and swelling.
If you are experiencing symptoms of chronic venous insufficiency, you can schedule an appointment with a vascular surgeon from our Division of Vascular and Endovascular Surgery at Jamaica Hospital in New York or learn more about the services at our vascular surgery center in New York. Please call 718-206-6713.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.



